Death. Morbid and depressing to most but a topic that fascinated me in college. A natural part of my everyday life. Before you report me to the Gardaí as a serial killer, zoom down to the microscopic level. Billions of our cells die everyday and many have been programmed to do so. A fine equilibrium is kept with new cells moving in to the vacant spaces. To find out what exciting developments are happening in this field of research, I caught up one of the most highly cited scientists in the world on programmed cell death, Prof. Seamus Martin of Trinity College Dublin.
It’s been 25 years since Martin began researching apoptosis after seeing an unusual morphology in the nucleus of Leukemic cells. After his PhD he made a deliberate switch to immunology and worked with the then emerging epidemic, HIV. He saw similar signs in HIV infected cells and was “dragged back into” apoptosis research. Martin explained that it is now known that “understanding cell death is fundamental to understanding diseases. In almost all major diseases you have a disturbance in cell death control. You either have too much cell death or too little cell death”.
Programmed cell death or apoptosis is effectively cellular suicide. Because of damage, old age or other circumstances, the cell initiates a set program that results in its death. Research in this area has been through its golden era of exploration. “It’s a good period in that we kind of understand the nuts and bolts of the process and that’s enabled to us to focus on what is really important”.
Developing Targeted Treatments
The central theme in apoptosis research is cancer as too little cell death results in a tumour. The mechanism of how this happens is now well understood so what is important to scientists at this stage is finding better targeted treatments. There are a number of key proteins involved in both initiating and preventing programmed cell death. Martin explains that “a lot of the focus right now is on trying to neutralise the pro-survivors of the BCL-2 family in cancer… because that effectively is what puts the brake on cell death”. These pro-survival proteins prevent the initiation of programmed cell death and tumours are often reliant in a mutation in one of these proteins for their continued survival. Neutralising these can tip the balance in favour of cell death.
One of the main challenges to cancer treatment is targeting the tumour and not promoting cell death in healthy cells in the body. Tumours are under intense pressure which is termed oncogenic stress. “It has evolved through this Darwinian process which means it has had to make a lot of compromises. This means it has a lot of addictions which it has traded in order to extend it’s survival”. These addictions are mutations in proteins such as members of the BCL-2 family. Targeting these altered molecules can enable tumours to more readily succumb to programmed cell death and will also have less impact on healthy cells.
Another class of compound, IAPs (inhibitor of apoptosis proteins), surprised many researching in this field. These proteins prevent some proteins, caspases, involved in apoptosis from working. It turns out that IAPs can be effective at promoting cell death in tumours. Why is this surprising? Scientists were puzzled as IAPs do not prevent apoptosis as they are part of a process downstream of the main suicide instructions. At that stage, cells are already doomed to die. After investigation “it turns out that with some tumour cells they are for some reason prone to killing themselves by upregulating TNF (Tumour necrosis factor)”. Their ability to increase the amount of this protein that promotes cellular suicide makes them perfect drug candidates and some are currently at the clinical trial stage.
Recruiting the Immune System
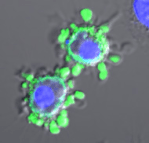
An exciting development in this field is the link between apoptosis and the immune system. The immune system is not activated in apoptosis which is a good thing as it results in the cell being disposed of without damaging surrounding cells. This is the major difference between programmed cell death and other types of cell death. Previously, it was thought that apoptotic cells were ignored by the immune system but recently this has been proven to be quite the opposite. “It looks like apoptotic cells are actively soliciting the help of the immune system to clear them and quite possibly also shutting down the aggressive microbe killing properties of the immune system”.
The ability for cells undergoing apoptosis to harness the immune system’s wound healing response is an exciting development and has implications for a new set of diseases. Harmful inflammation is associated with diseases such as rheumatoid arthritis and Crohn’s disease. “It seems that apoptosis may harness this wound healing response quite actively and that’s quite exciting because that may give us clues as to how we might use this information to manipulate the immune system in disease situations to harness a wound healing response and shut down the more inflammatory aggressive response”.
Martin published a paper a few years ago linking one of the proteins I mentioned earlier, caspases, to this immune system response. Caspases are involved in coordinating the demolition of the cell once programmed cell death has been activated. They are a key component in programmed cell death as they are “systematically shutting down the weapons at the cells disposal that could, if leaked out, activate the immune system”. Martin and his team showed that caspases inactivate a protein to prevent this immune response. The appropriately named protein, alarmin (or interleukin-33), is similar to a monitored alarm as when it’s turned on, the immune system police come with sirens blazing. Once caspases make a snip in its structure, it can no longer signal for help.
Linking Science & Industry
More recently, Martin’s lab have worked on another protein, interleukin-1 beta (IL1B), which acts in a similar way to alarmin. They discovered that “cell death related proteases trim off four amino acids from that protein to not only inactivate the protein but convert it to an antagonist to its own receptor”. Linking research and industrial application in a way that would make Science Foundation Ireland proud, they have patented this modified IL1B protein. This potential biopharmaceutical can prevent the production of the immune system recruiter IL1B. It may have applications in diseases such as rheumatoid arthritis and Crohn’s disease by reducing the harmful immune system response that underpins them. They are currently in talks with companies willing to take it to the clinical trial stage.
After chatting to Prof. Martin, I am even more fascinated by death of this kind. Now that the basic mechanisms are known, this field of research is becoming even more exciting. The hard work is beginning to pay off as science-based treatments are in various stages of development. An exciting chapter for apoptosis research!
Images: Courtesy of US National Library of Medicine (title) and the Molecular Cell Biology Lab, Trinity College Dublin (contents)
Lüthi AU, Cullen SP, McNeela EA, Duriez PJ, Afonina IS, Sheridan C, Brumatti G, Taylor RC, Kersse K, Vandenabeele P, Lavelle EC, & Martin SJ (2009). Suppression of interleukin-33 bioactivity through proteolysis by apoptotic caspases. Immunity, 31 (1), 84-98 PMID: 19559631
Martin SJ (2010). Cell biology. Opening the cellular poison cabinet. Science (New York, N.Y.), 330 (6009), 1330-1 PMID: 21127237
Other posts in this series:
- Science +1: Glimpsing at the frontier of science
- The search for life in the universe (by Markus Hammonds)
- Engage! (by Shaun O’Boyle)
- Small science with a big impact (by Dr. Éilis McGrath)
- Things are going to change around here! (by Humphrey Jones)
- The future of the Internet is wired into the human brain (by Prof. Billy O’Connor)

